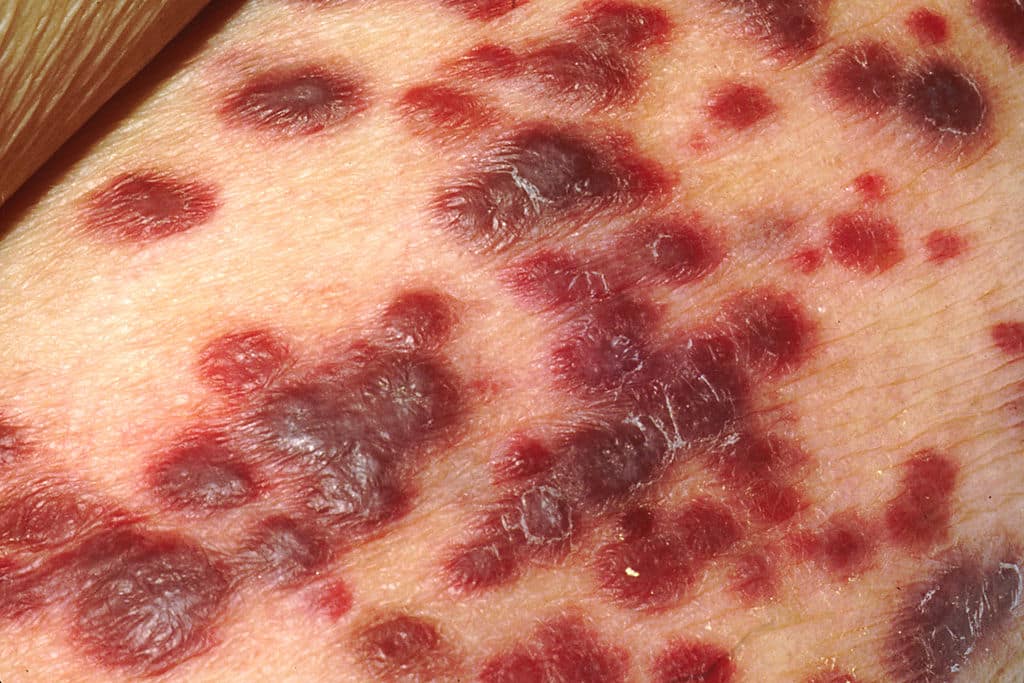
How to treat HIV/Aids
If you are diagnosed with HIV, then you need to start treatment as soon as possible to avoid replication and multiplication of the virus in your body and damaging the immune system. The good thing is that due to medical advancements and research, there are better HIV treatment options today than there were some years …