New HIV Testing Guidelines Released By WHO to Help Reduce HIV Prevalence and Improve Treatment Coverage
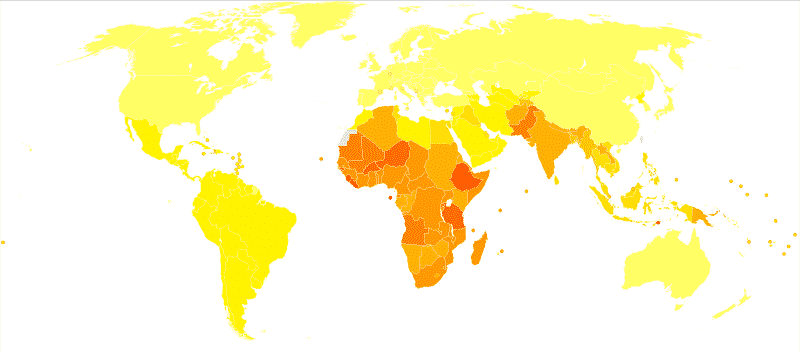
WHO is constantly working to provide better methods of eliminating the risk of the many dangerous STDs, especially in countries where the risk is at its peak, with Africa being one of them. Because of the high HIV rates, among other STDs in Africa, the WHO have decided on new guidelines that are believed to …