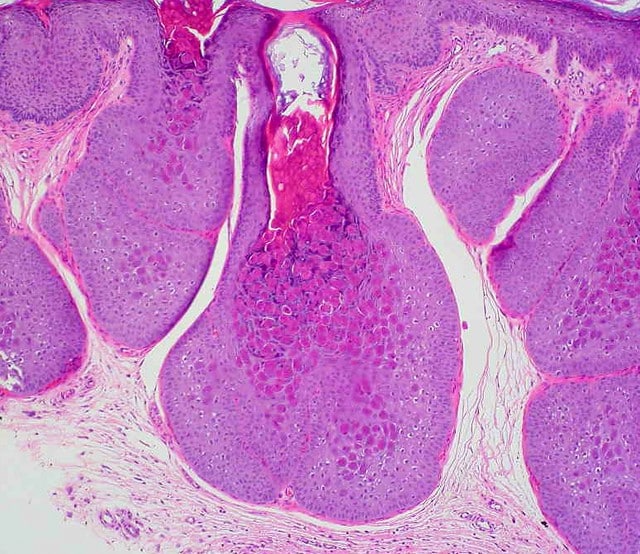
Molluscum Contagiosum in Africa
Africa has a warm tropical climate. Researchers have observed that molluscum contagiosum is more prevalent in warm climates with lightly dressed children. In Mali, the disease is among the common dermatoses in children. According to Medscape, child molluscum is prevalent in some regions of Africa like Papua New Guinea. More than 52% of children over …